To Inject Or Not To Inject?
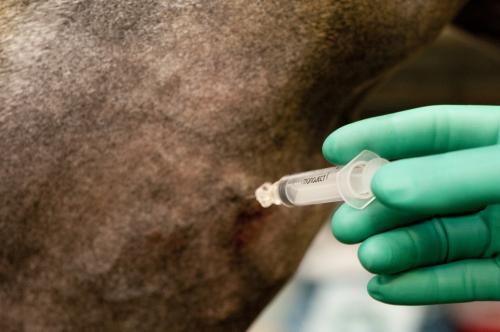
Joint (intra-articular (IA)) injections are often performed to treat joint inflammation and injury. This delivers treatment directly into the joint, ensuring the therapeutics are present where they are most needed, as opposed to systemic treatments (i.e. given intravenously, orally or intramuscularly) that have to travel through the body to the site of injury or disease.
Deciding which IA therapeutics to employ depends on multiple factors, including degree of lameness, specific joint, condition of that joint, horse’s age, riding discipline, veterinarian’s preferences and experiences, costs, and timelines. Accurate diagnosis prior to treatment is essential to ensure appropriate therapeutic intervention.
Some common IA therapies include:
Corticosteroids
If your horses receive IA injections, there’s a good chance they are getting corticosteroids. They are an effective, inexpensive, first-line approach to combating joint disease. Corticosteroids, including triamcinolone acetate (TCA), methylprednisolone acetate (MPA), and betamethasone acetate, are used for their anti-inflammatory effects. However, despite their popularity, IA corticosteroid use is controversial.
Research indicates that TCA protects cartilage and MPA can reduce signs of joint inflammation, and improvements in lameness have been observed with both. However, concrete evidence regarding efficacy is lacking. Harmful effects have been reported, with some being dose-dependent, and research on repeated injections of corticosteroids has suggested deleterious effects on cartilage. Corticosteroids can move from joint spaces to surrounding soft tissues and have been shown to delay healing, so they should not be used in horses with soft tissue injury.
Case reports suggest that corticosteroid administration is a possible risk factor for laminitis, but several studies have shown little evidence of association in healthy horses. Corticosteroid use should be avoided in geriatric horses and horses with metabolic disorders (EMS and PPID, for example) who are at increased risk for complications including the development of laminitis.
Overall, many questions about IA corticosteroid use remain unanswered and further studies are required.
IV & IM
Intravenous (IV) administration of HA is common, especially for less localized disorders. Only one HA product, Legend® (Bayer), is currently licensed for IV administration in horses in the U.S. Studies have reported decreased lameness in up to 90% of IV HA-treated horses.
Adequan® (American Regent Animal Health) is the only FDA-approved intramuscular (IM) polysulfated glycosaminoglycan (PSGAG) product for osteoarthritis in horses. Research has shown that the IM product can reach the joint where it may limit cartilage-degrading enzymes. Often used as a preventative measure, no scientific studies to date have investigated prophylactic use.
Hyaluronic acid/hyaluronan/hyaluronate (HA)
Naturally-occurring in synovial fluid and cartilage, HA is a viscous substance comprised of glycosaminoglycans (GAGs) that reduces friction in the joint. Concentration of HA decreases with age and inflammation makes joint fluid thinner and less protective. Injections are often used to treat inflammation, helping synovial fluid maintain a thicker, more protective consistency. It is most effective for mild to moderate levels of osteoarthritis (OA), but has limitations for treating more severe disease.
Biologics/Autologous Blood Products
Platelet-rich plasma (PRP)/Autologous conditioned plasma (ACP) – A cell-based therapy, PRP is made from the patient’s blood to contain a higher concentration of platelets than whole blood. Platelets are the first cells to respond to an injury. They contain growth factors and cytokines that promote healing and regulate inflammation. Platelet-rich plasma delivers high levels of growth factors and is used to treat musculoskeletal injuries and OA.
The effects of PRP on tendon and ligament injuries have been more thoroughly evaluated than its efficacy in joints. Results are promising, but strong scientific evidence to support the clinical use of PRP for joint disease is lacking. The composition of blood, including platelet concentration, varies by age, breed, and sex, which potentially influences the effects of PRP, and impacts how research studies are conducted and compared. These individual characteristics mean there are no standardizations for the preparation and application of PRP, so several methods have been described. Additional research and standardization are required to determine optimum dosing, timing and number of treatments across various injuries, tissue types, and surgical procedures.

Interleukin-1 receptor agonist protein (IRAP)/Autologous conditioned serum (ACS) – A cell-free product in which blood is incubated with specially designed glass beads to generate an enriched serum, IRAP is an anti-inflammatory that blocks interleukin-1 (IL-1), an important mediator of inflammation and joint degradation. To treat joint disease, IRAP is typically administered every seven to ten days for three to five treatments, although in cases of longer-term management of chronic joint disease, a single injection can be effective. It generally takes one day to process IRAP. Since it is a cell-free preparation, IRAP can be easily frozen and stored. It is particularly beneficial in cases of joint disease with concurrent soft tissue injury.
Stem cells – Regenerative therapies are primarily focused on cartilage regeneration by mesenchymal stem cells (MSCs). Although most studies have not demonstrated comprehensive cartilage regeneration, reduction of clinical signs and successful return to work have been reported. Outcomes and comparisons across studies and treatments are challenging as disease stage, number of cells, source of cells, culture techniques, implantation methods, and patient age and sex can significantly affect the function and efficacy of MSCs. Consequently, the ideal timing, number of cells, and recommended doses have not been established. Further studies involving stem cells in controlled models are required before this approach can be reliably employed to treat cartilage damage.
A wide variety of IA therapeutics have been evaluated in horses with joint disease, allowing for individualized approaches. Work with your veterinarian to select targeted approaches specific to your horse’s needs.
